Chronic kidney disease (CKD) affects multiple organs, including the skin. Many patients are surprised to learn that chronic kidney disease skin changes are extremely common and may even appear before severe kidney symptoms develop.
Skin symptoms such as itching, dryness, and discoloration are not just cosmetic concerns. They can indicate toxin buildup, mineral imbalance, or worsening kidney function.
What are the Skin Changes in CKD?
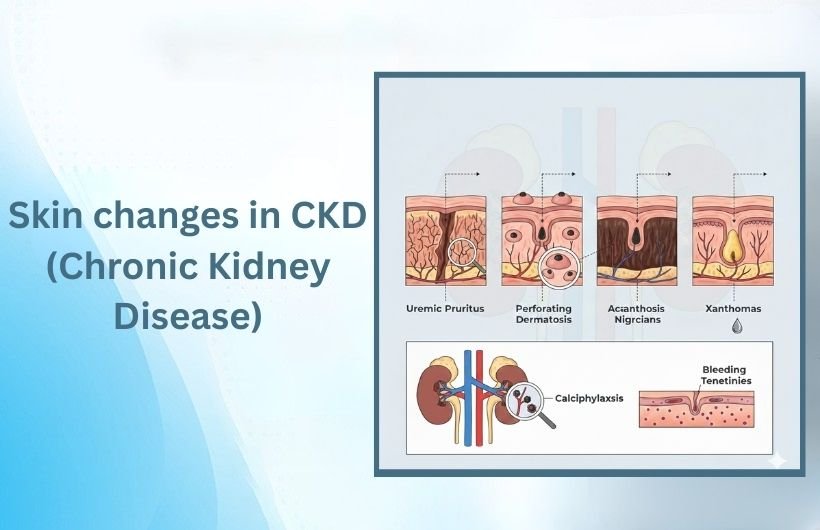
Skin changes in CKD include dry itchy skin (uremic pruritus), hyperpigmentation, pallor, rashes, thin fragile skin, easy bruising, and in advanced cases, uremic frost.
These occur due to toxin accumulation, fluid imbalance, anemia, and disrupted calcium-phosphorus metabolism.
Most Common CKD Skin Changes
1. Dry and Itchy Skin (Uremic Pruritus)
One of the most frequent CKD skin changes is persistent itching without a visible rash. This condition is known as uremic pruritus.
Why it happens:
- Waste buildup in the blood
- Nerve irritation
- Severe skin dryness (xerosis)
- Dialysis-related factors
Itching often worsens at night and may affect sleep and quality of life.
2. Skin Discoloration (Hyperpigmentation or Pallor)
Patients may notice:
- Greyish or yellowish skin tone
- Darkening (hyperpigmentation)
- Pale skin due to anemia
These chronic kidney disease skin changes occur because failing kidneys cannot remove toxins efficiently and may reduce red blood cell production.
3. Rashes and Red Patches
Mineral imbalance (especially calcium and phosphorus) can lead to:
- Red irritated patches
- Scaling
- Inflammation
- Increased sensitivity
These dermatological manifestations are more common in advanced CKD stages.
4. Thin, Fragile Skin & Easy Bruising
CKD can affect:
- Collagen production
- Blood vessel strength
- Nutritional balance
As a result, skin may become thin and bruise easily.
5. Uremic Frost (Advanced Kidney Failure)
In severe kidney failure, tiny white crystal-like deposits may appear on the skin.
This rare condition occurs when very high urea levels are released through sweat.
Why Does CKD Cause Skin Changes?
Healthy kidneys:
- Filter toxins
- Balance fluids
- Regulate electrolytes
- Maintain hormone balance
When kidney function declines:
1. Toxin Accumulation
Waste products circulate in the bloodstream and affect skin cells.
2. Fluid Imbalance
Dehydration or improper fluid regulation causes extreme dryness.
3. Mineral & Hormonal Disturbance
Imbalance in calcium, phosphorus, and vitamin D contributes to itching, scaling, and inflammation.
4. Anemia
Reduced erythropoietin production leads to pale skin.
The skin often reflects internal kidney health.
How Common Are Skin Changes in CKD?
Skin manifestations are very common:
- Up to 70–80% of CKD patients experience some skin symptom
- Itching is highly prevalent among dialysis patients
- Severity increases with CKD stage progression
Despite this, skin symptoms are often underreported during consultations.
Are Skin Changes a Sign of Worsening CKD?
Sometimes, yes.
Sudden worsening of:
- Severe itching
- Marked discoloration
- New rashes
- Persistent dryness
May indicate:
- Rising toxin levels
- Inadequate dialysis
- Progression of kidney disease
Always discuss new symptoms with your nephrologist.
How Are CKD Skin Changes Diagnosed?
Doctors evaluate:
- Medical history
- Physical examination
- Kidney function tests (creatinine, GFR)
- Electrolyte levels
- In rare cases, skin biopsy
Early detection improves comfort and quality of life.
Dr. Ravi Bhadania stresses that early detection allows better symptom management and improves quality of life.
Treatment for CKD Skin Changes
While underlying kidney disease may not be fully reversible, symptoms can be managed.
Medical Treatment May Include:
- Prescription moisturizers
- Anti-itch medications
- Topical corticosteroids (if needed)
- Dialysis adjustments
- Phosphate binders
- Nutritional correction
At-Home Skin Care Tips
- Use fragrance-free moisturizers daily
- Take short, lukewarm showers
- Avoid harsh soaps
- Pat skin dry instead of rubbing
- Follow prescribed fluid guidelines
- Protect skin from extreme weather
Consistent skincare can significantly reduce discomfort.
When Should You See a Doctor?
Seek medical advice if you notice:
- Severe persistent itching
- Skin infections
- Sudden color changes
- Bleeding under the skin
- Painful rashes
Early intervention prevents complications.
Conclusion
Skin changes in CKD are common but often overlooked.
Dryness, itching, discoloration, and rashes are not just cosmetic issues, they reflect internal kidney health.
If you live with chronic kidney disease and experience new or worsening skin symptoms, consult your nephrologist promptly. Early awareness leads to better symptom control and improved quality of life.
Understanding your body is the first step toward managing CKD effectively.
If you are experiencing CKD skin changes or other kidney-related symptoms, consult Dr. Ravi Bhadania, a trusted Nephrologist in Ahmedabad, for expert evaluation and personalised treatment guidance.
FAQs
Can CKD skin changes be cured?
They can be managed effectively. Proper treatment and kidney care can significantly reduce symptoms.
Does dialysis improve itching?
Dialysis helps remove toxins, which may reduce itching. However, some patients still require additional skin treatments.
Why is my skin itchy without a rash?
This is called uremic pruritus. It occurs due to toxin buildup and nerve irritation rather than surface inflammation.
Are CKD skin changes dangerous?
Most are not life-threatening but may indicate worsening kidney function. Sudden changes should always be evaluated.
Can lifestyle changes improve CKD skin problems?
Yes. Gentle skincare, mineral balance through diet, proper hydration (as advised), and medical follow-up help significantly.